

Vynca’s ECM program delivers compassionate, team-based support to help Medi-Cal members with complex needs navigate care and access resources to stay healthier.
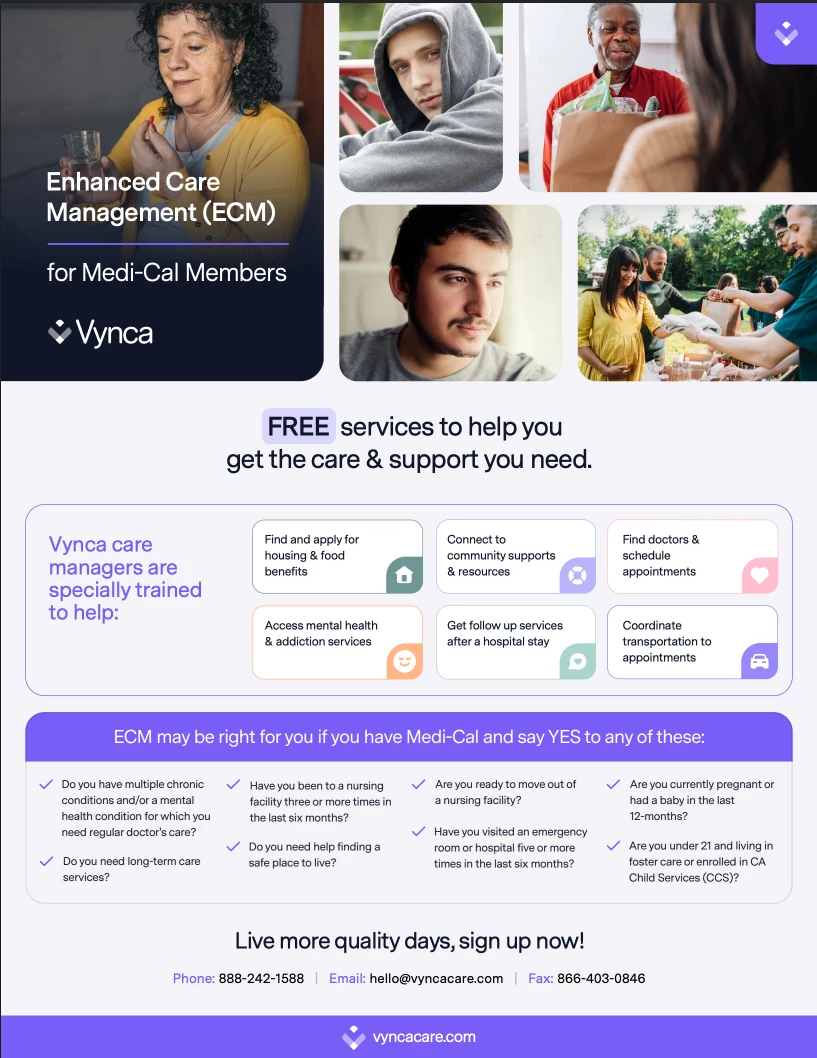
Enhanced Care Management is designed for people who
need more than traditional care coordination.
Vynca supports Medi-Cal members across [b]eight
populations of focus[b], including individuals who are:

This is proactive, relationship-based care — focused
on stability, dignity, and long-term outcomes.
Vynca’s ECM care team is specially trained to address both [b]medical and social
needs[/b], working closely with members to build trust and momentum.
Our support may include:
Vynca is a trusted ECM provider across California, serving
members through multiple Managed Medi-Cal plans.



















Personalized, no-cost support to help navigate
care, access resources, and move forward.
A trusted partner to support complex patients
beyond the clinic — without added burden.
Vynca Community Uplift Network (VCUN)

No single organization can meet every need alone. Through the Vynca Community Uplift Network (VCUN), we partner with trusted community-based organizations to identify, educate, and connect individuals who may qualify for ECM — creating faster access to care and stronger community ties.
Vynca is here to help.
Enhanced Care Management is a covered service that helps California residents enrolled in Medicaid who need extra support to stay healthy. Our staff works with you to make sure you get the right care and needed services.
Our goal is to make your life a bit easier and healthier by giving you the exact help you need, one step at a time.
Yes, Enhanced Care Management (ECM) services are covered for those enrolled in Medicaid plans that Vynca works with.
No. We work with your doctors to support you.
No. You can keep your current providers.
Please fill out a simple form with some details about you. We will check your health plan coverage and then help schedule your first visit.
We’ll check if you qualify for our program. Once this is a go, we’ll schedule your first visit with a member of our care team. We will ensure you have adequate access for virtual visits. We can provide smartphones or tablets and internet access for those who qualify.
To qualify for Enhanced Care Management (ECM) services, you typically need to meet certain criteria based on your health and social needs. While specific requirements can vary by program or location, here are some common factors that may qualify you:
Chronic Health Conditions: You may qualify if you have multiple chronic conditions such as diabetes, heart disease, or asthma.
Behavioral Health Needs: Individuals with mental health or substance use challenges may be eligible for ECM services.
High Risk of Health Issues: If you have frequent hospital visits, emergency room stays, or are at risk for serious health problems, you may be eligible.
Social Needs: People who face challenges like homelessness, lack of stable housing, food insecurity, or difficulty accessing care may qualify.
Referral: In many cases, a doctor, nurse, or social worker may refer you to ECM services based on your needs.
To find out if you qualify, you can apply today.
Yes. We talk with your doctors, share care information, and ensure we work together.
Yes. A physician referral is not required. Although, we might need approval from your health plan based on your benefits and coverage. If this is the case, we will let you know.